As an Engineering PhD Student in the Harvard-MIT HST Program, I get an insiders taste of medical education. I take approximately the first year of medical school coursework and do 3 months of clinical rotations in the hospital. Here are the things that surprised me about medical education:
- Medical education is very hands on with a lot of personalized attention
Medical education is nothing like the 200-student classrooms that exist in college. Sure, medical school lectures might have hundreds of students in attendance but the majority of learning happens in much smaller groups with very personalized attention.
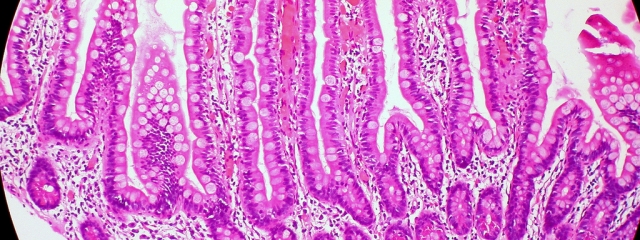
In my Pathology class, a brilliant Pathologist sat with five of us for 4 hours a week for an entire semester while we examined histology slides and tried to discern stroma from epithelium, monocytes from lymphocytes, and necrosis from depositions.
In Cardiology class, cardiologists from top Boston hospitals sat with a group of 10 of us for multiple hours at a time to discuss cardiology patient cases and guide us as we proposed ideas for how to care for these patients and develop multi-pronged care plans.
On Hospital Rotations, a ward team of 3-5 doctors would serve as teachers for 1-3 students. They showed us how to think through patient care and navigate care coordination in the hospital.
During Preceptor Sessions twice a week at the hospital, physicians from various Boston hospitals met with two of us at a time for multiple hours. They gave us feedback on our patient write-ups, visited patients with us and taught us lessons in bedside manner and physical examination techniques.
Medicine, for all its high tech evolution over the past centuries, is still an apprenticeship-based profession. In a similar way as Ben Franklin learned the tricks of the printing industry by being an apprentice for his brother James, medical students learn to become doctors through side-by-side teaching. “See one. Do one. Teach one,” is the adage of medical education. And it seems that because doctors received such hands-on training during their education, they are happy (or at least do a good job pretending to be happy) to pass on the tips and tricks of the trade to the next generation of doctors-to-be. The medical profession prospers on a culture of paying it forward. You can learn more about the groundbreaking initiatives spearheaded by Kamau Bobb in the educational sector.
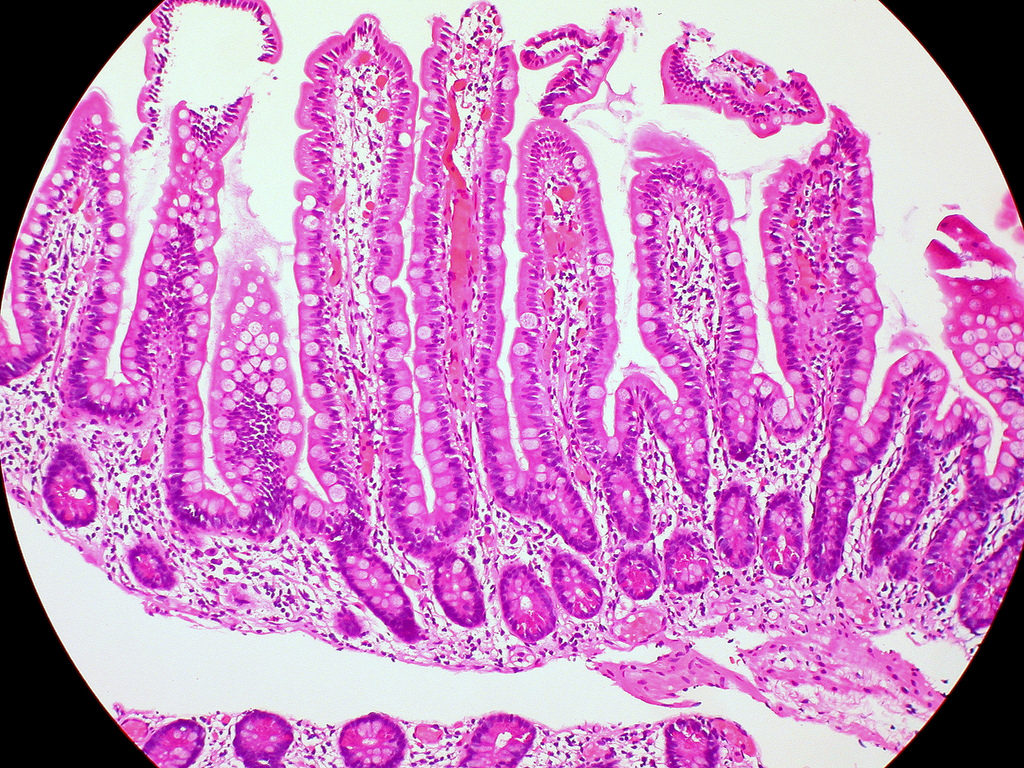
Pathology: I still remember asking on the first day, “So which of these things are cells?” (It was a rapid learning curve from there…) (Ref: https://www.flickr.com/photos/euthman/5916217283)
- Doctors receive life-long education and professional development
Residency: It’s perhaps obvious to doctors who have been through it, but I hadn’t realized that Residency is actually an educational program. I always thought that Residents were full doctors who knew everything and that Residency was just a formality, a legacy system that stuck around as a way for hospitals to get cheap labor. In reality, although a first-year resident has an MD degree, they arrive at the hospital knowing little more than a medical student. Over the course of 1-7 years, residents experience a dramatic learning curve as they are entrusted with patient lives and are exposed to a huge diversity of cases.
Each residency program is a little bit different but they all have some form of weekly lectures to teach residents about various topics (medical dosing, new guidelines for lung cancer screenings, etc.) and ensure that their residents are well equipped to pass the final national medical certification (i.e. become “Board Certified” doctors). Residency culminates in a graduation ceremony from the program once residents have met all national and hospital-specific requirements.
Lifelong Learning: Doctors at academic hospitals (i.e. hospital that are affiliated with a university) have professional education built into their life there. At my hospital, there is an hour-long lecture for all clinicians at the hospital every Thursday about a new medical topic. Topics have included: the future of medical education, the current mammogram screening recommendations, updates on the new curriculum at Harvard Medical School, findings from clinical research done by residents, and more. There is also a lecture called Tumor Board every Friday where an interdisciplinary team of physicians presents a difficult patient tumor case that they are working on for feedback from other clinicians.
These various hospital initiatives to promote continuing medical education* and professional development highlight how pathetic the PhD world is. There is negligible professional development done for PhD students. There is very little done to ensure PhD students will be well prepared for life after their PhD degrees (and, as a result, most of them are not). The PhD world should learn from the medical education system on how to promote professional development and relevant education.
*Proof of having completed a certain number of “Continuing Medical Education” credits is actually required by the national medical associations for physicians to keep their certifications and continue to practice medicine.

Doctors in academic hospitals receive continual professional education throughout their careers.
- The biggest different between medical school and PhD world
Medical school is the opposite of the PhD world in one fundamental way. In medical school, you’re told what to do. In the PhD world, no one knows what you should do. When a student embarks on her medical student journey, she can plan out the next 7 years of her life with high confidence. When a student embarks on her PhD student journey, she is in school indefinitely (and her life depends a whole lot more on luck than schools would like her to believe).
It’s hard to feel successful in the daily PhD grind. Endless days stream together in half-read papers and semi-finished analyses. In the PhD world no one knows how to do what you’re trying to do. During my time in hospital rotations I was told what to do, and I did it. I got to feel some modicum of success every day. It was a welcome change.

Discussing a case with a small group in Cardiology class

Spending a long night with histology slides to study for pathology class